Living with Parkinson’s leg pain can feel frustrating, tiring, and even scary at times. Legs may ache, cramp, feel stiff, or burn without warning, making daily activities harder than they should be. The good news is that there are natural, practical ways to reduce discomfort and regain confidence in movement while supporting overall health.
In this guide, we explore gentle strategies to ease Parkinson’s leg pain, including exercise and therapy, medical guidance, and lifestyle changes. With the right plan and support from Shadowleaf at Estrella Gardens, managing pain becomes more achievable and less overwhelming.
Understanding Parkinson’s leg pain
Understanding why Parkinson’s leg pain happens is the first step toward relief. Pain in Parkinson’s disease is common and can come from several sources, including muscle stiffness, nerve changes, and involuntary muscle contractions known as dystonia. Many people experience pain after prolonged sitting or during specific movements.
A key question families often ask is what causes pain in Parkinson’s patients. Pain may stem from reduced dopamine levels, which affect muscle control, posture changes, and nerve signaling. Over time, these issues can interfere with daily comfort and mobility.
Triggers can vary from person to person. Some people feel worse pain in the morning, while others notice discomfort after activity. Gentle stretching and awareness of these triggers can help reduce flare-ups. Support services such as senior respite care also play an important role by giving caregivers time to recharge while loved ones receive attentive care.
Why medical guidance matters
Pain should never be ignored, especially when it changes suddenly. Consulting a healthcare provider helps ensure that Parkinson’s pain treatment is safe and personalized. Doctors assess pain severity, identify underlying causes, and rule out unrelated conditions like arthritis or circulation issues.
Medical evaluations also help clarify what causes pain in Parkinson’s patients as the condition progresses. In later phases, symptoms may overlap with Parkinson’s disease stages of dementia, requiring a more comprehensive approach to care.
For trusted resources, families can explore guidance from organizations like the Parkinson’s Foundation and the Michael J. Fox Foundation. These sources explain pain symptoms and treatment options in clear, helpful language.
Local support services, such as essential guidance for senior medical care, can also help families navigate appointments, medications, and care decisions.
Over-the-counter options for mild discomfort
For mild to moderate Parkinson’s leg pain, over-the-counter medications may help when used correctly. These options are widely available and can offer temporary relief.
Common choices include:
- Acetaminophen for general pain relief
- Ibuprofen to reduce inflammation
- Naproxen for longer-lasting relief
- Aspirin for mild discomfort
Always consult a healthcare provider before starting any medication, as interactions can occur with Parkinson’s prescriptions. Maintaining high-quality healthcare services ensures that pain relief choices remain safe and effective as part of a broader Parkinson’s leg pain treatment plan.
Prescription support for severe pain
When pain becomes intense or persistent, prescription medications may be necessary. These are often used when Parkinson’s pain treatment needs stronger support than OTC options can provide.
Doctors may recommend:
- Medications combining acetaminophen with codeine for musculoskeletal pain
- Gabapentin or duloxetine for nerve-related discomfort
Understanding risks is essential, as some medications can cause drowsiness or dependency. As Parkinson’s disease stages dementia advance, careful monitoring becomes even more critical.
Assisted living communities, such as those offering assisted living options in Arizona, provide medication management and daily support to help residents stay comfortable and safe.
Complementary therapies that support comfort
Massage therapy benefits
Massage therapy is a gentle yet powerful option for easing Parkinson’s leg pain. Techniques like Swedish massage or deep tissue therapy help relax tight muscles, improve circulation, and reduce stiffness.
Massage also supports emotional well-being by reducing anxiety and improving sleep quality. When combined with other forms of Parkinson’s leg pain treatment, massage can significantly improve daily comfort. Always work with therapists experienced in Parkinson’s care to ensure safety.
Why movement matters
Exercise is one of the most effective natural tools for Parkinson’s pain treatment. Regular movement helps maintain strength, balance, and flexibility while reducing rigidity and cramps.
Low-impact activities include:
- Walking
- Swimming
- Chair-based exercises
- Light strength training
Exercise may also slow symptom progression and support cognitive health during the stages of Parkinson’s disease and dementia. Many families turn to physical therapy programs recommended by the National Institute on Aging for guidance on senior-friendly movement.
Lifestyle changes that reduce pain
Small daily changes can make a big difference in managing Parkinson’s leg pain. Consistency matters more than intensity.
Helpful strategies include:
- Diet adjustments: Focus on anti-inflammatory foods such as fruits, vegetables, whole grains, and omega-3-rich fish.
- Hydration habits: Drinking enough water supports muscle function and circulation.
- Sleep routines: Quality rest improves pain tolerance and energy levels.
Stress management also plays a role in answering what causes pain in Parkinson’s patients, as anxiety can worsen muscle tension. Relaxation techniques like breathing exercises or guided meditation can help.
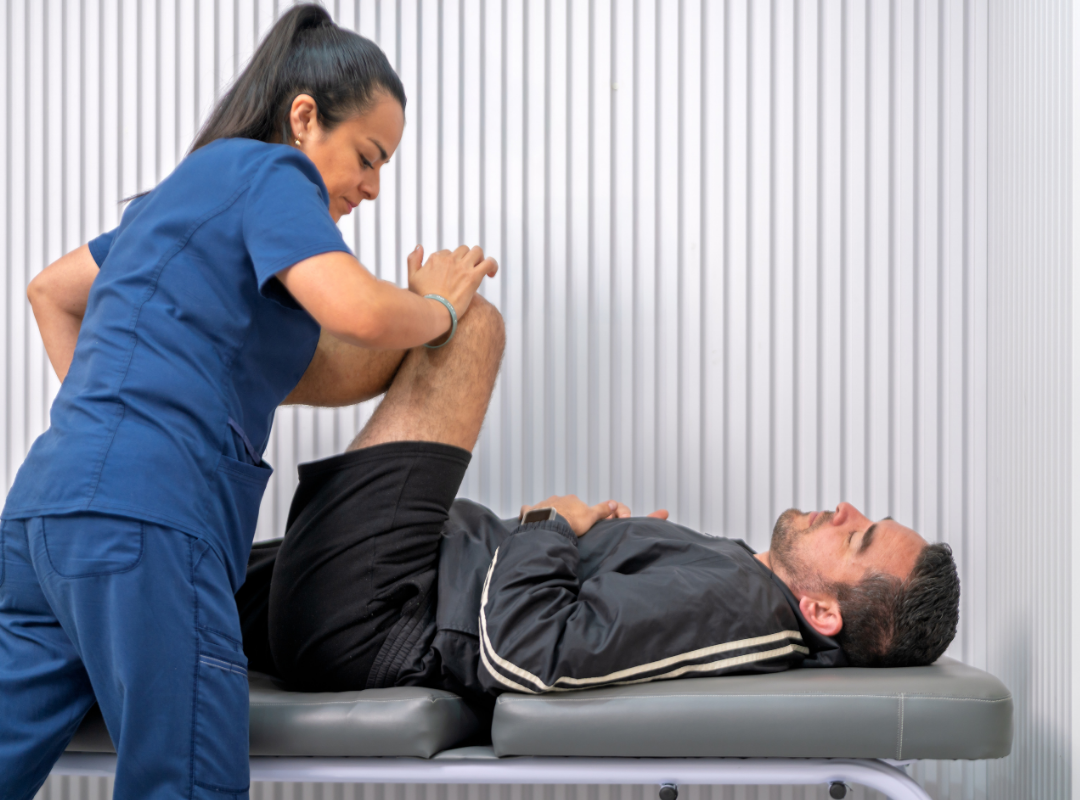
Exercise and physical therapy together
Combining exercise with physical therapy creates a strong foundation for managing Parkinson’s leg pain. Physical therapists design personalized programs that improve mobility while reducing discomfort.
| Exercise Type | Benefit | Frequency |
| Stretching | Improves flexibility | Daily |
| Strength training | Builds muscle support | 2–3 times weekly |
| Aerobic activity | Enhances heart health | 150 minutes weekly |
| Balance exercises | Reduces fall risk | 2–3 times weekly |
These routines not only ease pain but also improve confidence and independence, even during later Parkinson’s disease stages and dementia.
Understanding pain across Parkinson’s stages
Pain can change as Parkinson’s progresses. Early on, discomfort may be mild and occasional. Later, Parkinson’s disease stages dementia may bring communication challenges that make pain harder to express.
Care teams must watch for nonverbal cues, such as facial expressions and changes in movement. This awareness helps ensure that Parkinson’s pain treatment remains responsive and compassionate at every stage.
Talk to us about lasting relief
Let’s Help You Find Comfort Again
Living with Parkinson’s leg pain does not mean giving up comfort, movement, or joy. With the right mix of medical guidance, natural therapies, and daily support, relief is possible.
At Shadowleaf at Estrella Gardens, we specialize in compassionate care that adapts to every stage of Parkinson’s. Call us today at 702-577-2637 to learn how our community can support you or your loved one. Ready to experience peace of mind in a caring environment? Schedule a tour here and let us walk this journey with you.
Frequently Asked Questions
What is the average life expectancy of a Parkinson’s patient?
The average life expectancy of a person with Parkinson’s disease is often similar to that of the general population, especially with early diagnosis and proper care. Many individuals live 15 to 20 years or longer after diagnosis. Life expectancy can vary depending on age at diagnosis, overall health, and how well symptoms are managed. Complications such as falls, infections, or swallowing difficulties can impact longevity, making ongoing medical care necessary.
How does Parkinson’s start?
Parkinson’s disease usually begins gradually, often with very mild symptoms that may go unnoticed at first. Early signs commonly include a slight tremor in one hand, stiffness, or subtle changes in movement and posture. Some people experience non-motor symptoms early on, such as loss of smell, sleep disturbances, or constipation. Because symptoms develop slowly, diagnosis often occurs after noticeable changes in movement appear.
What is a nursing diagnosis for Parkinson’s disease?
A nursing diagnosis for Parkinson’s disease focuses on how symptoms affect daily functioning and safety. Common diagnoses include impaired physical mobility, risk for falls, self-care deficit, and impaired swallowing. Nurses also consider cognitive changes, communication difficulties, and emotional well-being when planning care. These diagnoses help guide personalized care plans that support independence and quality of life.
What are the signs that Parkinson’s is getting worse?
Signs that Parkinson’s disease is progressing often include increased tremors, worsening stiffness, and slower movement. Balance problems and frequent falls may become more common as the condition advances. Non-motor symptoms such as memory issues, mood changes, hallucinations, or sleep problems may also intensify. As symptoms worsen, individuals may require more assistance with daily activities and personal care.

